What is the gut microbiome?
The gut microbiome is a bustling ecology of microorganisms that reside in our digestive tract. It is composed of a wide array of bacteria, viruses, fungi, and other microscopic organisms that play a vital role in our overall health.
While the gut microbiome is unique to each individual, there are certain commonalities that can be found among healthy individuals.
It is estimated that the human body contains approximately 37 trillion human cells, while the gut microbiome consists of 100 trillion microbial cells. This number is two and a half times greater than the number of human cells in the entire body. This means that our bodies are, in terms of cell count, more microbial than human.
All those trillions of microbes inhabit the entire gastrointestinal (GI) tract, from the mouth to the colon, forming a dynamic and complex ecosystem that plays a crucial role in digestion.
The journey of microbes in our gastrointestinal (GI) tract begins from the moment we take our first bite. As we chew our food and mix it with microbes in the saliva from our mouth, we introduce bacteria into our system. These bacteria then travel down the esophagus and into the stomach, where they encounter a harsh environment of stomach acid. However, some bacteria are able to survive this acidic environment and continue their journey.
Once in the small intestine, the bacteria find a more favorable environment. The small intestine provides nutrients and a mucus lining that allows the bacteria to thrive. As the food passes through the small intestine, the bacteria continue to break down complex carbohydrates and other substances.
As the food reaches the large intestine, the number and diversity of bacteria increase. This is where the majority of our gut microbiome resides. The large intestine provides a suitable environment for bacteria to flourish, with its warm temperature and availability of nutrients.
Throughout the entire GI tract, the microbes adhere to the intestinal lining and form biofilms, which are communities of microorganisms. These biofilms protect the bacteria from being washed away by the passing food and provide a stable environment for them to live.
In the colon, the final section of the GI tract, the bacteria play a crucial role in fermenting undigested carbohydrates and producing short-chain fatty acids. These short-chain fatty acids are important for maintaining the health of the colon cells and regulating inflammation.
Why does gut microbiome matter?
A healthy gut microbiome is characterized by a diverse population of microorganisms associated with health. As mentioned earlier, these microorganisms work together to digest complex carbohydrates and fibers that our bodies can't break down on their own. When you consume foods like whole grains, vegetables, and legumes, your gut microbiome plays a crucial role in fermenting these indigestible components into short-chain fatty acids (SCFAs) like butyrate, acetate, and propionate. SCFAs serve as an energy source for the cells lining the colon, helping to maintain the health of the gut lining, have anti-inflammatory properties and also play a role in regulating metabolism and appetite.
Your microbiome also plays a pivotal role in regulating immunity. In fact, approximately 70% of our immune system is located in our gut. Your gut acts as a training ground for immune cells, teaching them to distinguish between harmful pathogens and beneficial microbes. Certain gut microbes also produce essential nutrients like vitamins (e.g., B vitamins and vitamin K) and amino acids that are necessary for various physiological processes in the body such as balanced metabolism, nerve function, blood clotting, and bone health.
How do we maintain microbiome stability?
Maintaining a good condition of microbiome composition is crucial for our overall health and well-being. Despite the constant influx of new bacteria and other microorganisms, our gut microbiome has mechanisms in place to maintain a relatively stable composition in healthy adults. That stability is maintained firstly through a combination of competition among microorganisms. In a healthy gut, there is a stable ecosystem that makes it difficult for harmful organisms to dominate. Additionally, the gut environment itself plays a role in maintaining stability via temperature, pH levels, oxygen levels and more. The gut provides an ideal environment for the growth of certain microbes while being less conducive to the growth of others. Microbiome stability can be also maintained through a balanced diet rich in fiber, diverse food choices, and probiotic and prebiotic foods.
Understanding and maintaining microbiome stability is pivotal for overall health and well-being, and this knowledge forms the foundation for emerging personalized health approaches like microbiome-based diets.
Microbiome and personalized nutrition
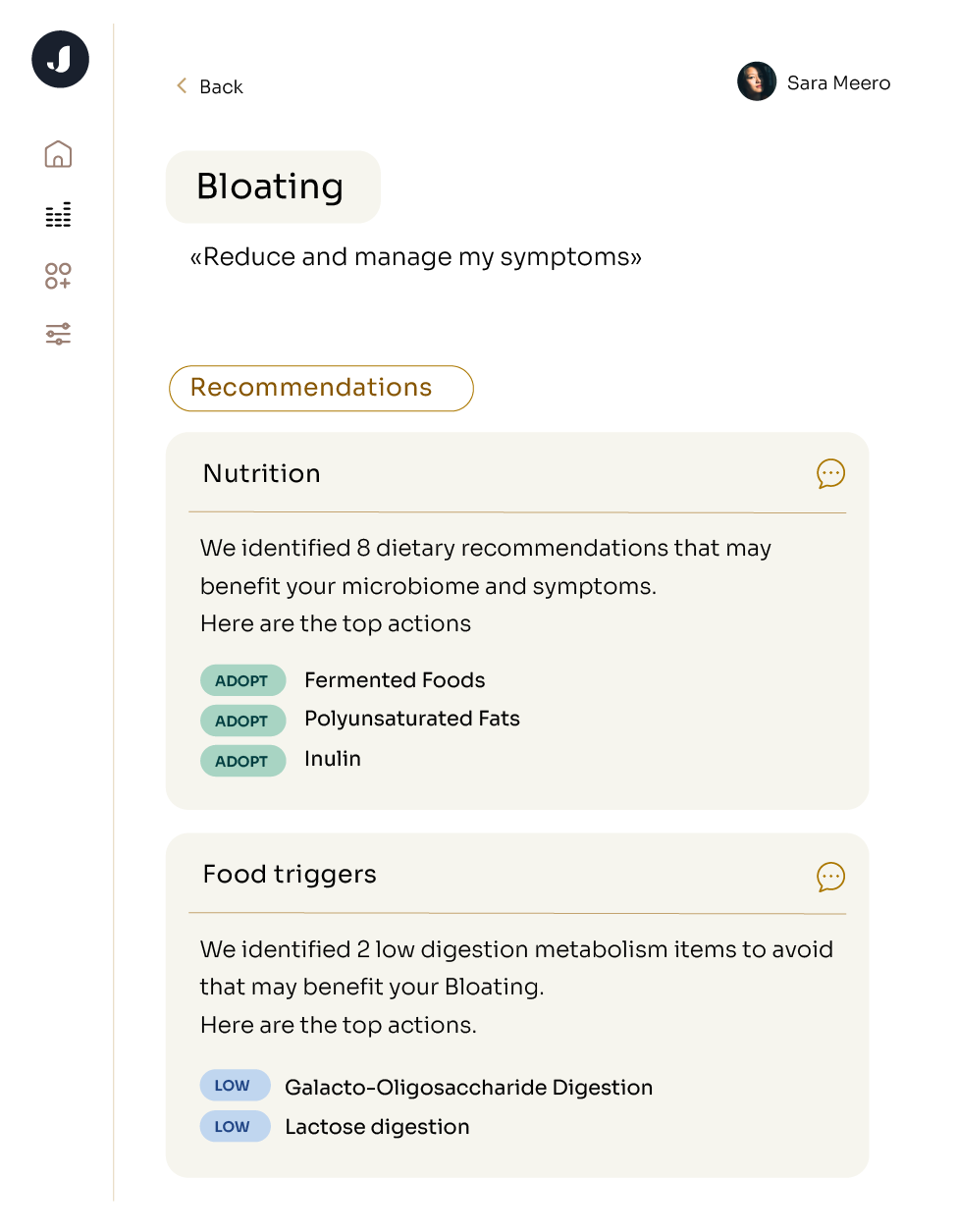
Understanding the specific makeup of an individual's microbiome can potentially allow for personalized health and nutrition approaches. Personalized diets based on the gut microbiome, often referred to as "microbiome-based diets" or "precision nutrition," are an emerging area of research and health optimization. These diets are based on a microbiome analysis which is done through techniques like metagenomic sequencing, which provides information about the types and relative abundance of microorganisms in the digestive tract. The microbiome data is then used to profile the individual's gut microbiota, including the presence of specific bacterial species, diversity, and functional capacity. This profile can be linked with the literature to understand how the microbiome is affecting health and how dietary changes can steer the microbiome in a target direction. The goal for these procedures is to see specific microbial patterns that have been associated with health conditions and to make dietary recommendations to improve the microbiome associated with these conditions. Individuals following personalized microbiome-based diet may undergo regular monitoring of their gut microbiome to assess how dietary changes are affecting their microbial composition and overall health, adjusting their diets accordingly.
The idea behind these diets is to tailor dietary recommendations to an individual's unique gut microbiome composition and activity to improve certain aspects of their health. By analyzing a person's microbiome, healthcare providers can offer targeted recommendations for diet, probiotics, and medical treatments to optimize health outcomes. This approach may revolutionize how we approach healthcare by recognizing the "one-size-fits-all" model of dietary changes doesn't apply to everyone.
Microbiome associations to health conditions
When our gut microbiome is disrupted, it can lead to a condition known as gut dysbiosis. Research has linked gut dysbiosis to conditions such as obesity and type 2 diabetes as changes in the composition of gut bacteria can affect the metabolism of dietary nutrients, leading to increased inflammation and insulin resistance. Additionally, a dysbiotic microbiome may influence the storage of fat and energy extraction from food. Furthermore, the gut microbiome influences our mental health. Recent research has shown a strong connection between the gut and the brain, known as the gut-brain axis. A healthy microbiome helps produce neurotransmitters, such as serotonin, which is often referred to as the "feel-good" hormone. In fact, more than 90% of serotonin is synthesized in the gut. Imbalances in the gut microbiome have been linked to mental health disorders like anxiety and depression where research indicates a potential role for certain genera of bacteria, such as Bifidobacterium and Lactobacillus, in promoting mental well-being. Moreover, the association between imbalances in the gut microbiome and the development of neurodegenerative diseases like Parkinson's or Alzheimer’s has been found. A decrease in Prevotellaceae and an increase in Enterobacteriaceae, have been observed in individuals with those diseases. These changes are thought to potentially contribute to the neuroinflammatory processes associated with the condition.
Is also worth highlighting that the gut microbiome plays a role in modulating the immune system, which can impact the body's ability to recognize and control cancer cells. Dysbiosis may contribute to chronic inflammation, which is a known risk factor for cancer development. Additionally, researchers discovered that hormonal fluctuations, particularly in women's health, can influence the gut microbiota, and conversely, the gut microbiota can impact hormone metabolism. Dysbiosis may play a role in conditions like polycystic ovary syndrome (PCOS) and hormonal imbalances. Gut health can also affect estrogen metabolism, potentially influencing conditions related to estrogen, such as endometriosis.
Additionally, the gut-skin axis is a topic of particular interest for scientists. This concept suggests a connection between gut health and skin conditions. Gut microbiota dysbiosis may contribute to skin problems like acne, eczema, and psoriasis. Inflammation triggered by imbalances in the gut microbiome can manifest as skin inflammation. There are several bacteria crucial to maintaining a healthy skin condition and one of them are Firmicutes and Bacteroidetes. An imbalance between Firmicutes and Bacteroidetes has been associated with conditions related to systemic inflammation, which could potentially affect the skin. Furthermore, Akkermansia muciniphila has been associated with the gut mucosal layer and has been linked to gut health. Changes in its abundance have been observed in various health conditions such as psoriasis, and it may have broader implications for systemic inflammation and skin health. Additionally, some strains of Bifidobacterium are considered beneficial probiotic bacteria and have been associated with anti-inflammatory effects. Modulating the balance of Bifidobacterium in the gut may have implications for immune system regulation, which could impact skin conditions.
Understanding the gut microbiome is crucial for maintaining our general health and well-being. By promoting a healthy microbiome through proper nutrition and lifestyle choices, we can support our immune system, improve digestion, and enhance overall health. Profiling your individual microbiome is a powerful tool for gaining insights into your gut health and its potential connections to various conditions and symptoms. It enables personalized healthcare, helps identify dysbiosis, uncovers triggers, guides targeted interventions, allows for progress monitoring, and contributes to ongoing research efforts. To learn more about the link between gut microbiome and different conditions we recommend following the Jona blog where we cover these topics in more detail.